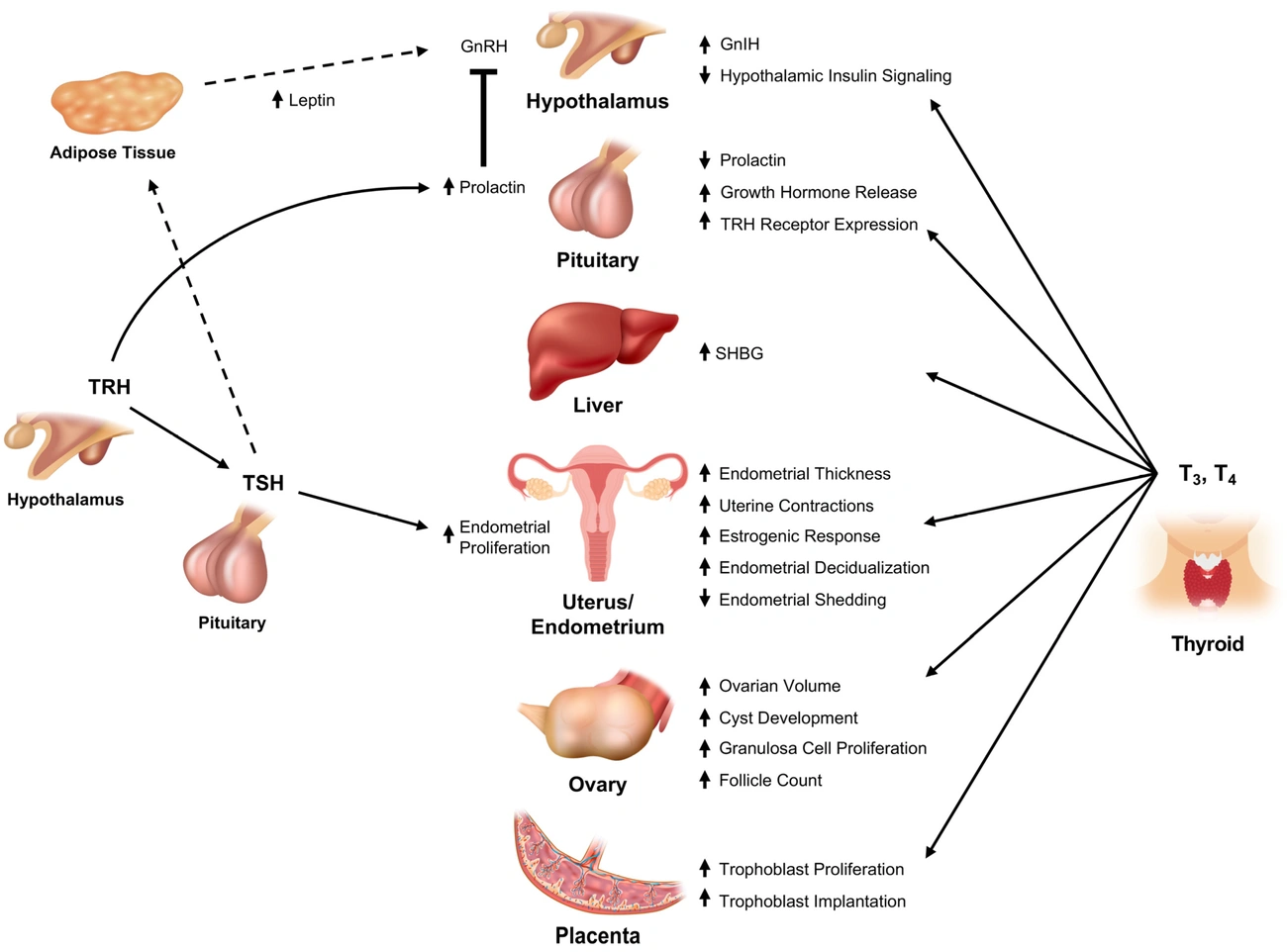
PCOS and Thyroid Problems: What Your Doctor Isn’t Telling You
PCOS and thyroid problems occur together far more often than most women are told. Autoimmune thyroid disease affects nearly one in four women with PCOS, compared to fewer than one in twenty women without it. Yet in routine clinical practice, thyroid health is rarely discussed during PCOS treatment.
This oversight creates a dangerous loop. Thyroid dysfunction worsens insulin resistance, weight gain, fatigue, and fertility issues—exactly the symptoms women with PCOS are already battling.
The Overlooked Link Between PCOS and Thyroid Problems
Research consistently shows that women with PCOS have more than double the risk of developing thyroid disorders over time. Autoimmune hypothyroidism, especially Hashimoto’s thyroiditis, is dramatically more common in PCOS.
The reason lies in shared root causes:
- Insulin resistance driving hormonal imbalance
- Chronic low-grade inflammation
- Increased body fat and estrogen dominance
- Genetic susceptibility affecting endocrine organs
When doctors treat PCOS without assessing thyroid health, they miss a critical piece of the puzzle.
How Thyroid Dysfunction Worsens PCOS Symptoms
Thyroid hormones regulate metabolic rate, glucose handling, fat breakdown, and reproductive hormone balance. Even mild hypothyroidism slows metabolism and intensifies insulin resistance—fueling PCOS progression.
Insulin Resistance: The Common Enemy
Low thyroid function reduces glucose uptake in muscles and increases glucose output from the liver. This worsens insulin resistance, a core driver of PCOS. The result is stubborn weight gain, higher androgen levels, and worsening cycle irregularity.
The Estrogen–Progesterone–Thyroid Triangle
PCOS often leads to estrogen dominance and progesterone deficiency. Excess estrogen increases thyroid hormone binding proteins, reducing the amount of active hormone reaching cells. Low progesterone further impairs thyroid efficiency, creating a hormonal bottleneck.
Symptoms That Should Raise Red Flags
Because hypothyroidism and PCOS share symptoms, thyroid issues are often dismissed as “just PCOS.” Warning signs include:
- Persistent fatigue despite lifestyle changes
- Weight gain resistant to diet and exercise
- Hair thinning on the scalp with increased facial hair
- Cold intolerance and low energy
- Irregular periods or infertility despite treatment
Why Standard PCOS Treatments Often Fail
Birth control pills regulate bleeding but do not correct insulin resistance or thyroid dysfunction. Metformin targets blood sugar but does nothing for thyroid autoimmunity or hormonal imbalance.
This is why many women feel “stuck”—labs look acceptable, but symptoms persist.
Why Thyroid Testing Is Non-Negotiable in PCOS
Basic TSH testing alone is insufficient. Women with PCOS frequently have subclinical hypothyroidism that goes undetected unless a full thyroid panel is done.
A proper evaluation should include:
- TSH
- Total T3
- Total T4
Identifying thyroid dysfunction early can prevent worsening PCOS symptoms and long-term metabolic damage.
A Root-Cause Strategy That Helps Both Conditions
1. Nutrition That Lowers Insulin Resistance
A low-glycemic, high-protein, healthy-fat diet improves insulin sensitivity and reduces inflammation—benefiting both PCOS and thyroid health.
2. Strength Training Over Cardio Alone
Resistance training 3–4 times weekly improves glucose uptake, reduces androgen levels, and boosts metabolic rate. Muscle acts as a glucose sink, reducing insulin burden.
3. Stress and Sleep Optimization
Elevated cortisol worsens thyroid conversion and PCOS symptoms. Consistent sleep and stress reduction are essential for hormonal recovery.
4. Strategic Supplement Support
Myo-inositol improves insulin sensitivity and ovulation. Vitamin D reduces inflammation and supports immune balance. Magnesium, zinc, and probiotics further enhance metabolic and hormonal health.
Final Verdict: Treat the System, Not the Symptom
PCOS and thyroid problems are not separate diagnoses—they are interconnected metabolic and hormonal disorders. Treating one while ignoring the other leads to partial results at best.
True healing begins when insulin resistance, thyroid health, inflammation, and lifestyle are addressed together. This integrated approach is what creates lasting symptom relief, hormonal balance, and improved fertility.
Frequently Asked Questions
Can thyroid problems cause PCOS?
Thyroid dysfunction does not directly cause PCOS but can worsen insulin resistance and hormonal imbalance, triggering PCOS-like symptoms.
Should all women with PCOS get thyroid tests?
Yes. Women with PCOS have a significantly higher risk of thyroid disease and should undergo full thyroid testing, not just TSH.
Does treating hypothyroidism improve PCOS?
Correcting thyroid dysfunction often improves menstrual regularity, insulin sensitivity, energy levels, and fertility outcomes in women with PCOS.
Related Redial Programs
- PCOS Management Program
- Diabetes Reversal
- Obesity Reversal
- Hypertension Reversal
- Lifespan Extension
- Anti-Cancer Diet Support
References
Medical Disclaimer: This content is for educational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider before making any changes to your medication, diet, or treatment plan. Individual results may vary.